Diagnosis
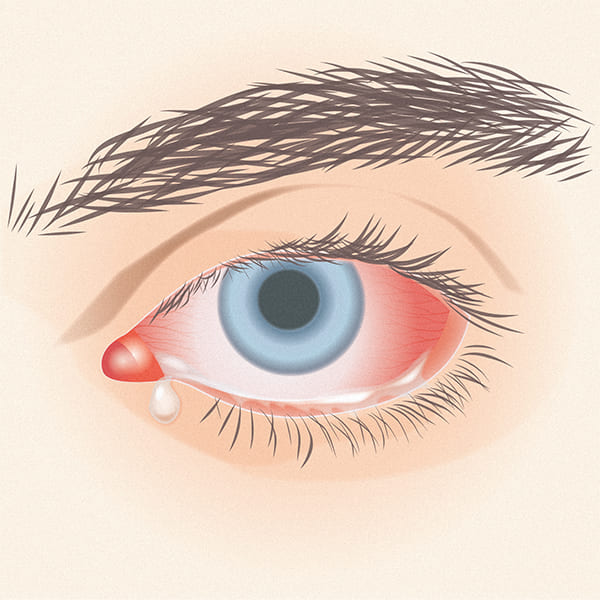
The diagnosis of allergic conjunctivitis is made by the ophthalmologist, following an assessment of the symptoms and the appearance of the eye (eyelid swelling, hyperaemia, chemosis, papillary reaction).
The specialist may also examine the eye with a special instrument, the slit lamp, which allows him or her to detect any signs of allergy (such as dilated blood vessels on the eye surface).
Treatment
Treatment for allergic conjunctivitis usually involves the use of antihistamine and anti-inflammatory eye drops on prescription. The use of artificial tears is also important, both for their power to wash away and dilute the allergens present on the eye mucous membranes, and because they can improve symptoms if refrigerated. Finally, careful cleaning of the eyelids and eyelashes is recommended (preferably without detergents, perhaps with saline solution) to remove allergens that may be deposited there.
Since the allergic predisposition of each individual generally persists throughout life, in the treatment of allergic conjunctivitis it is important to first remove or avoid as far as possible the responsible allergen. This can be done, for example, by avoiding areas where grass is being cut, or going to the countryside at certain times of the year, or, in the case of mite allergies, by eliminating objects that trap dust in the house and washing bed linen at a temperature above 50°.