Bacteria and health
We are used to seeing our bodies as a single entity that belongs to us alone; in reality, each human body is home to numerous micro-organisms, to the extent that the number of foreign microbial cells is much higher than the number of our own cells.
The skin can be regarded as an ecosystem composed of different habitats and niches that support a wide range of microorganisms, including bacteria, fungi and viruses. This community of microorganisms that we all live with is called the microbiota.
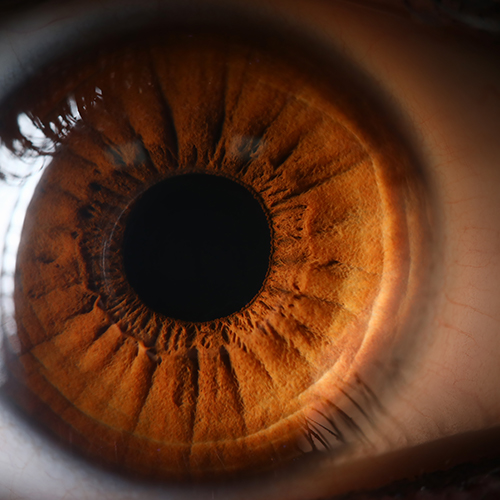
Compared to other areas of the human body, there are far fewer bacteria present in the eye area. This is due to the presence of powerful antimicrobial factors in the tear film and the continuous mechanical action of the eyelids, which sweeps away microbes. Despite this, many microorganisms survive on the ocular surface.
The microbiota of the eye is characterised by bacteria that do not normally cause infection or inflammation. On the contrary, these bacteria contribute to good ocular health by blocking the growth of pathogens through a competition mechanism. In addition, the interaction between our microbial flora and the cells of the eye creates “immunological tolerance”, whereby our immune system learns not to attack the “good” bacteria in the ocular microbiota, but at the same time learns to recognise and attack the “bad” ones.
Several studies have been carried out to characterise the microbial community in the eye area, i.e. to determine which bacterial species live in this area of the body and in what quantity. Specifically, on the eyelids and conjunctiva (the thin membrane covering the front surface of the eye) the most common species of microorganisms are Staphylococcus aureus, coagulase negative staphylococci including Staphlylococcus epidermidis, Propionibacterium acnes and corynebacteria.

Changes in the microbiota and eye diseases
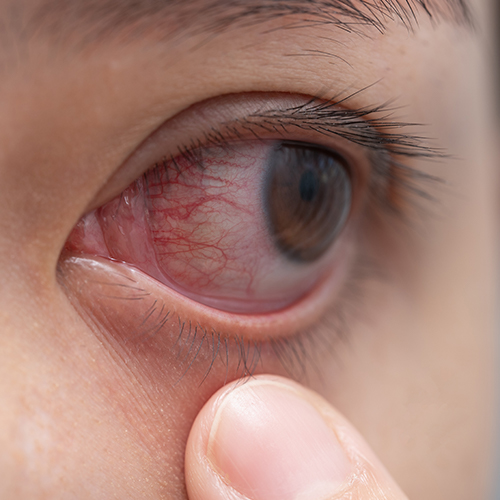
Knowing the characteristics of our “resident” microbial community is important for the treatment and prevention of some common eye diseases, including blepharitis and dry eye disease. Changes in the composition of the ocular microbiota have been observed in these and other diseases, and it is not yet clear whether this change is the cause or a consequence of the disease. Wearing contact lenses also changes the ocular microbiota, with different effects depending on age, lens type and frequency and duration of use.
In blepharitis patients, the bacterial presence is generally higher than in healthy controls. In particular, corynebacteria emerged as the most common micro-organisms in blepharitis sufferers (54% of cases), followed by Staphylococcus epidermidis (35% of cases) and Staphylococcus aureus (13% of cases). These bacterial strains appear to be actively involved in the development of blepharitis. The Demodex mite also appears to play a role in the onset of chronic blepharitis, as well as in conjunctival inflammation and dysfunction of the Meibomian eyelid glands.
Dysfunction of the Meibomian eyelid glands can lead to a decrease in the oily component of tears, causing increased evaporation of the tear film and subsequent development of dry eye disease. The secretions of the Meibomian glands are characterised by a complex composition and a high number of bacteria. In cases of dysfunction of these glands, the complexity of microbiota composition and bacterial abundance increases with increasing disease severity: the severity of eyelid gland dysfunction is strongly correlated with an altered ocular microbiota.
Eyelid hygiene has been proposed as a preventive approach to reduce ocular bacterial load without significantly affecting the diversity of species residing in the eye area. In particular, the application of an ophthalmic spray containing 0.01% hypochlorous acid can significantly reduce the microbial load without altering the diversity of bacterial species in the eye area. Consequently, this spray may be useful in the management of blepharitis, Meibomian gland dysfunction, dry eye disease and other forms of eye irritation.
The influence of the gut microbiota on eye health
A balanced gut microbiota is a key factor in maintaining the optimal balance of the entire body, including the eye and its structures. According to the latest scientific research, an imbalance in intestinal bacterial strains, known as dysbiosis, can lead to chronic degenerative eye diseases such as glaucoma, uveitis and macular degeneration.
How this happens is now the subject of much research, but some hypotheses have already been put forward: when the microbiota is in dysbiosis, there is an increased production of inflammatory molecules that affect target structures at a distance. The presence of inflammatory substances alters the function of the immune system of all mucous membranes, including the conjunctival mucosa in the eye. In this context, any situation in which the immune system is impaired also involves the eyes.
Many studies are still needed to fully understand all the interactions that exist between the microbiota and the gut-eye axis, but this research will undoubtedly help us to identify new strategies for the prevention and treatment of numerous eye diseases soon.




How do you rate your experience on our site?
Comments
You need to log in to post a comment
No comments inserted